How It Works
Booking a scan with us is simple and easy, select your scan type and body parts, choose a date and time that works for you, and complete your booking.
Our expert team will check all of your details and confirm your booking, if there are any problems at all one of our friendly booking team will contact you.
During your scan, our expert radiologists will guide you through every step of the process and answer any questions you may have.
Once your scan is complete your results will be sent to your nominated consultant along with a copy being sent to you for your records.
Our scanning services
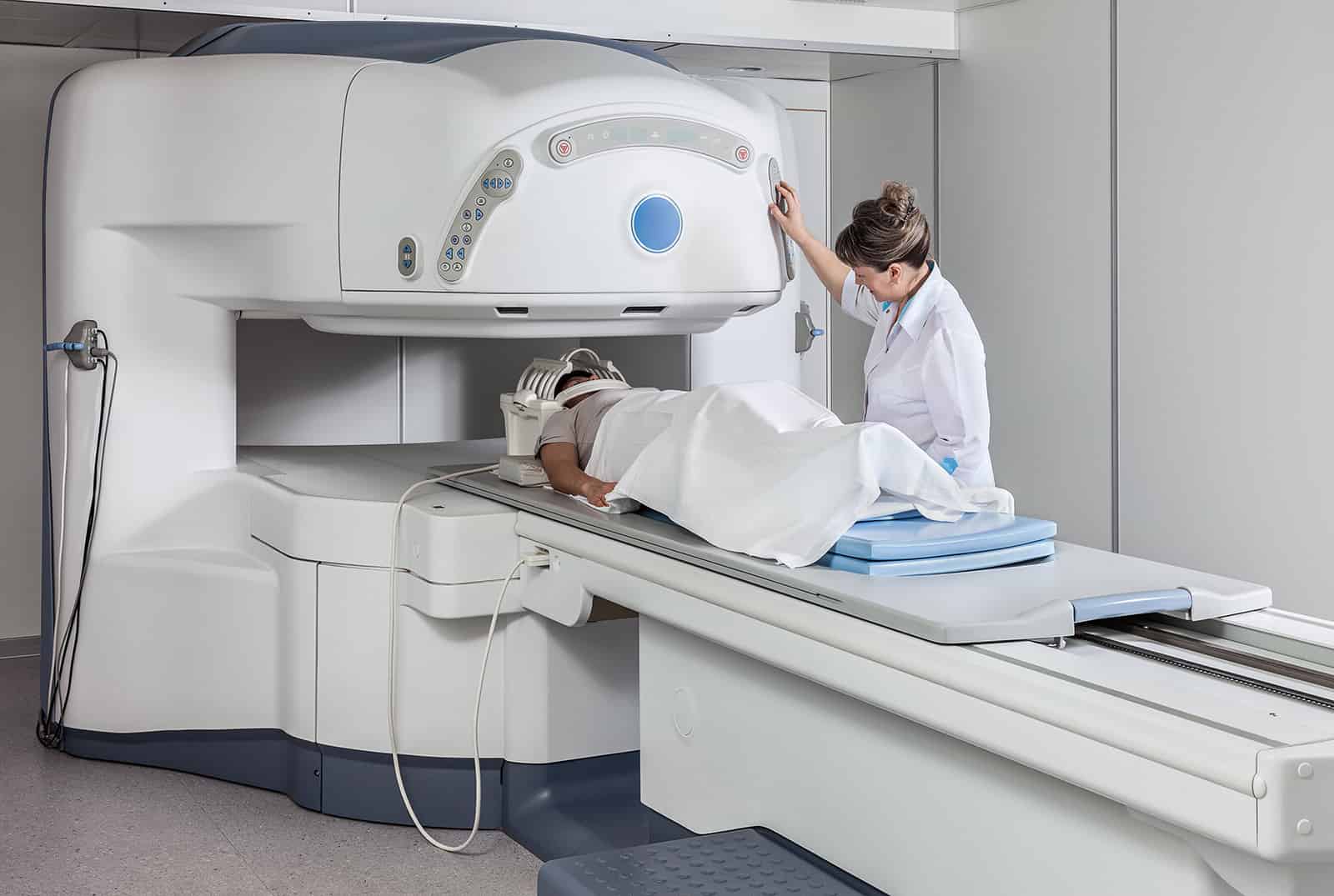
The open MRI uses a magnet on top and bottom and is open on all four sides. These decrease the risk of claustrophobia and panic attacks exponentially and allow patients of all shapes and sizes to be able to make use of an MRI to accurately diagnose their problems.
Read more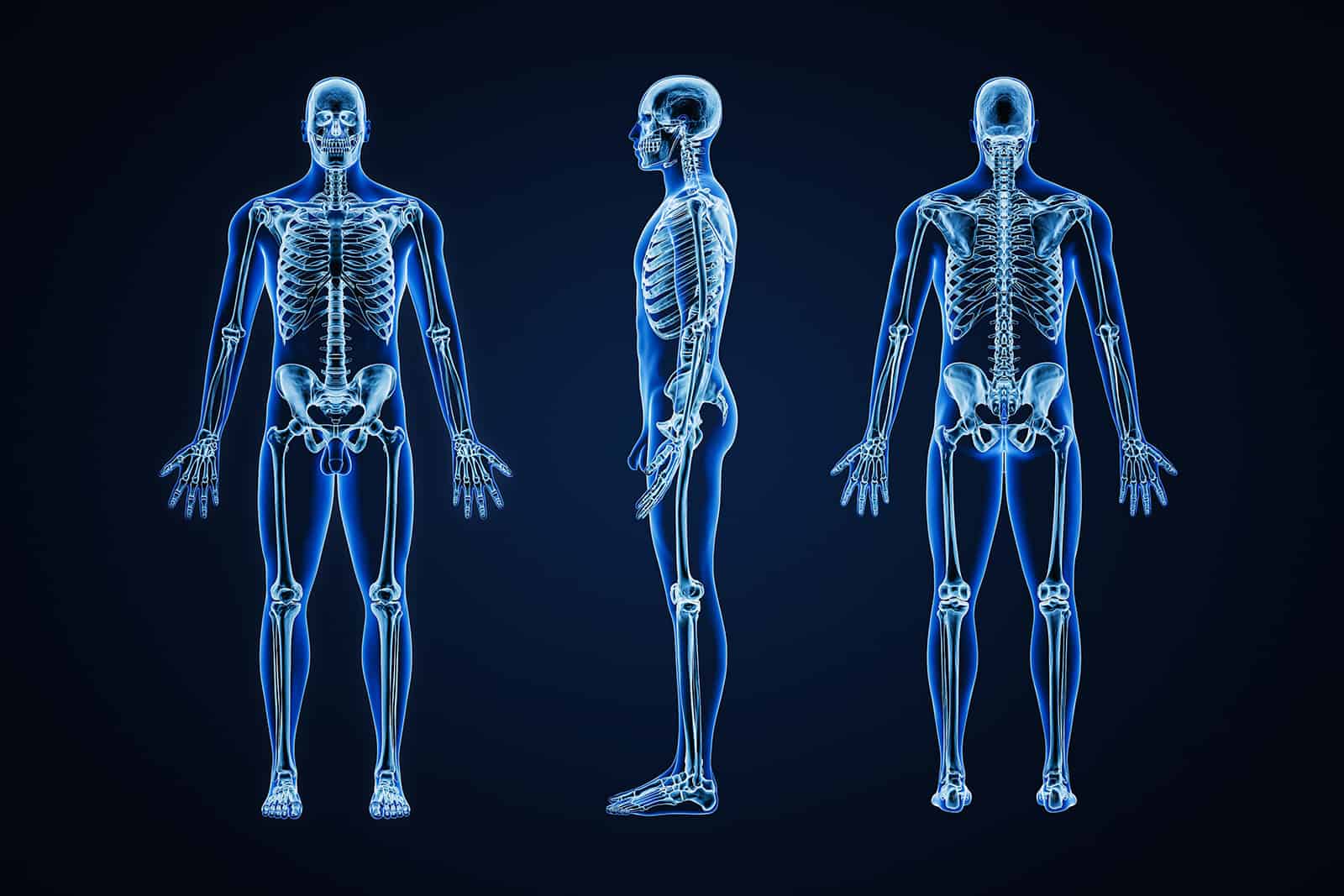
One scan, Multiple organs, Looking for potential cancer and disease indicators, our full body MRI scan provides a deep insight into your overall health.
Read moreThree ways to pay
No referral needed, your scan, when you want it.
MRI Plus is recognised by most major insurance companies.
MRI Plus are approved MRI Scan service providers to the NHS.